Sore throats are very common in winter and are usually caused by a virus that will get better by itself.
Occasionally, a sore throat with fever may be caused by a type of bacteria called Group A Streptococcus (also known as Group A Strep or GAS in short). GAS has been around for years, and many children will have been exposed to it already.
In fact, many of us, including children, carry it around normally without it causing any problems. However, very young children (under 5 years) may not have come into contact with GAS before because they have had less social mixing than usual because of the Covid-19 pandemic and subsequent lockdowns. This may be why so many children under 5 years are now contracting the bacteria.
Many get only mild symptoms with it or may have it without even knowing it and it doesn’t cause any problems. Some children may need simple oral antibiotics for it and a smaller proportion may need hospital treatment.
Luckily, complications from this disease are still very rare but parents and carers are extremely worried because GAS has been in the news because it has been the cause of some children becoming very ill and some sadly dying.
- Most commonly, children with GAS will have a sore throat and a fever.
- They will have yellowish-white spots at the back of their throat (their tonsils) and may have red spots at the top of their mouth (their palate).
- They may complain of pain in their neck, or you may notice that they have tender lumps (lymph nodes) in their neck.
- They usually don’t have much of a cough or a runny nose.
Some children with GAS develop Scarlet Fever where the children will have the same sore throat and a fever but also have:
- a sandpaper-like rash
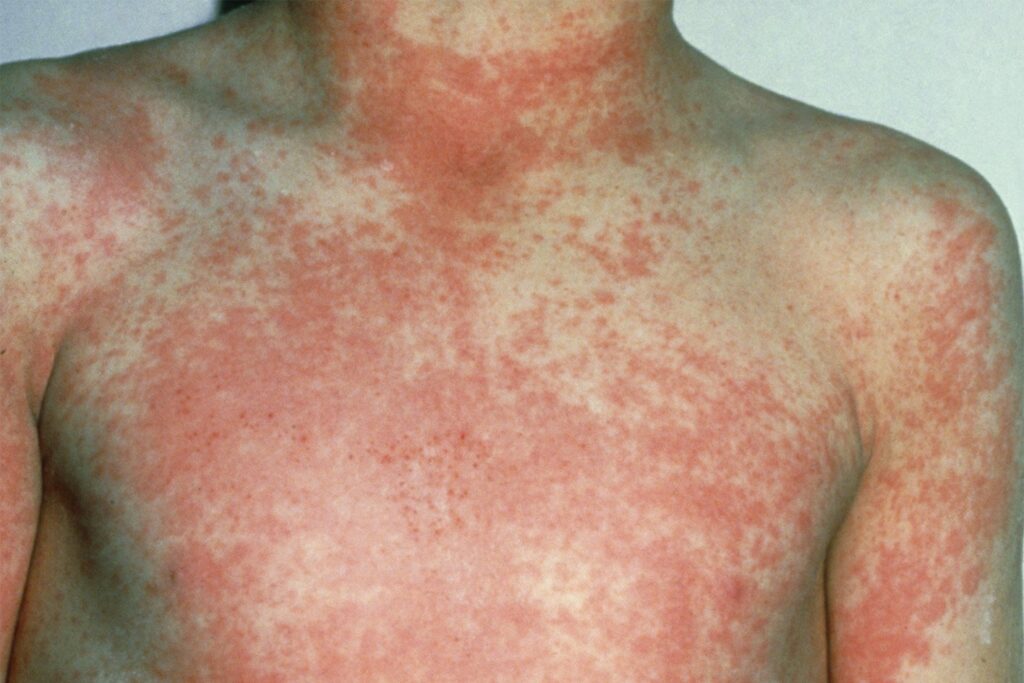
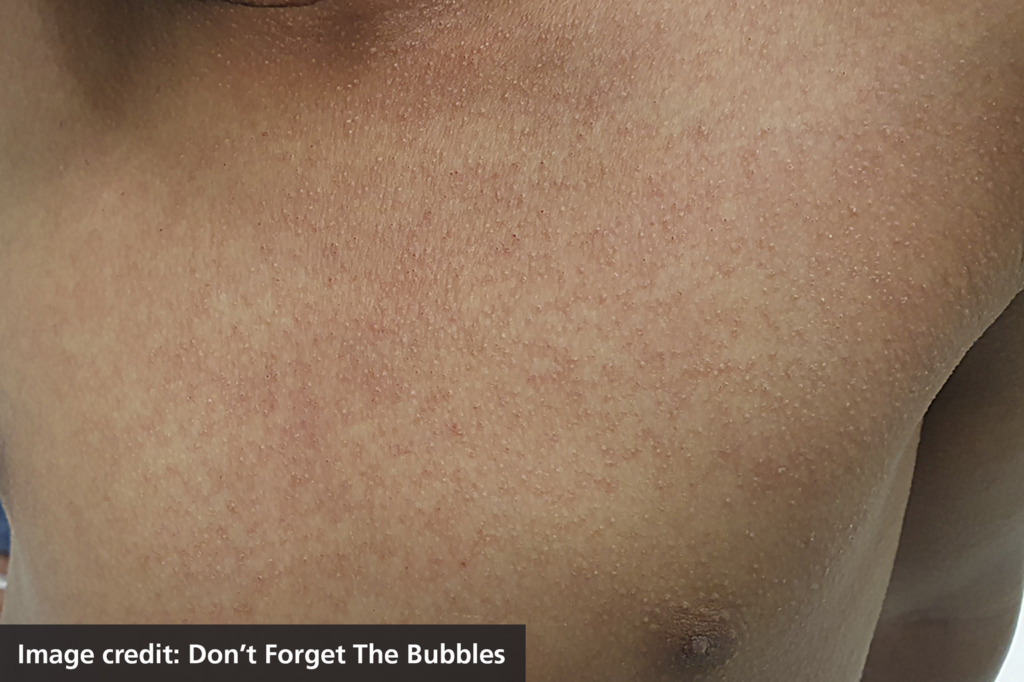
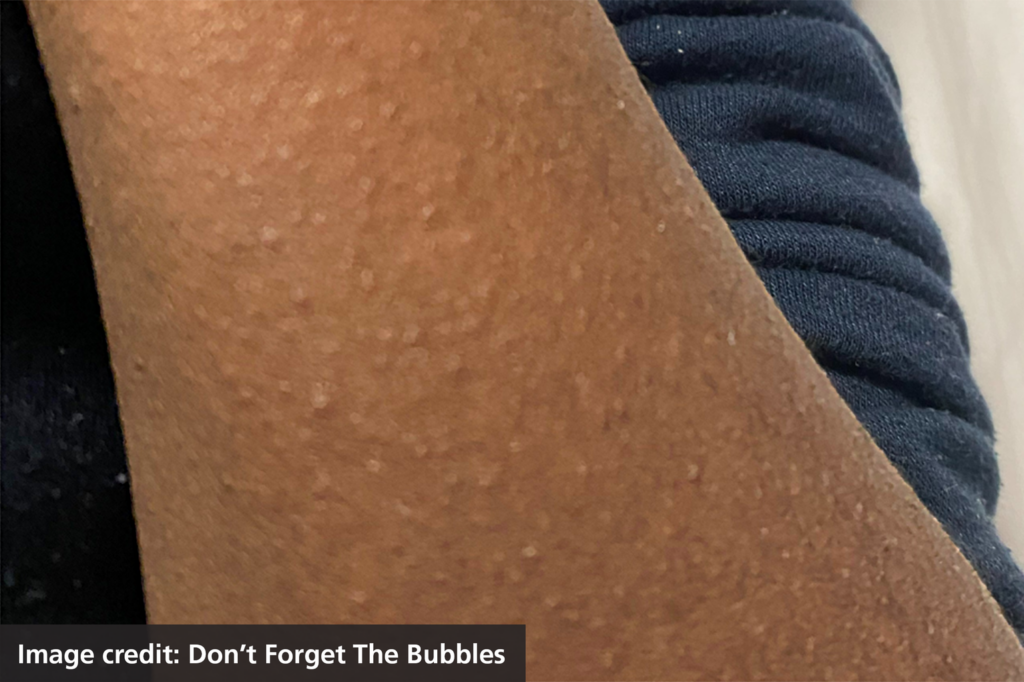
- very red lips or a red tongue
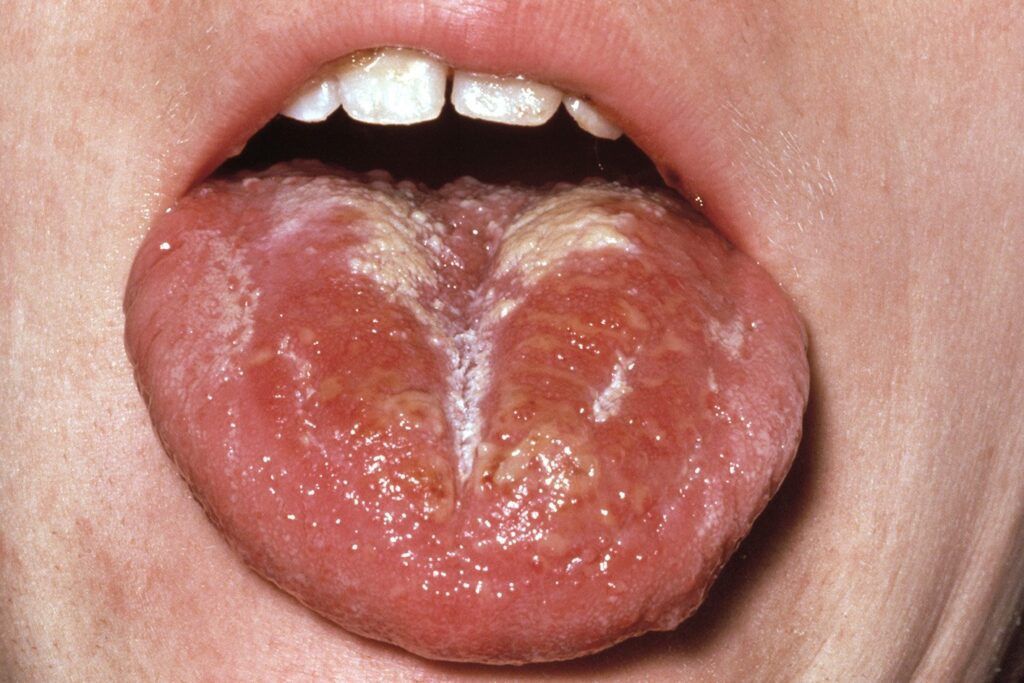

(Image credit to NHS Conditions and Don’t Forget the Bubbles)
Children with symptoms of GAS or Scarlet Fever will usually need treatment with antibiotics.
A very small number of children will develop complications from this disease. This includes:
- difficulties breathing
- dehydration
- painful limbs and joints
- very tender skin redness which spreads quickly.
If you notice any of these signs, especially if your child has been diagnosed with GAS, please use our checker to identify where you should take them to be reviewed.
Many of the complications arise because of a recent viral infection which makes the body weaker when fighting this opportunistic bacterial infection. Therefore, you can protect your child by making sure they are up to date with all their immunisations and have had their annual flu vaccination if they are over two years old.
Keep unwell children off school or nursery and away from vulnerable adults and children. If they have been diagnosed with GAS, they are to remain isolated for at least 24 hours after starting antibiotic treatment.
When should I worry and what should I do?
Call 999 or go to A&E now if your child:
Your child is having difficulty breathing
You may notice grunting noises or their tummy sucking under their ribs/the notch at the bottom of their neck pulling in and out or they are using their neck muscles to breathe
There are long pauses (more than 10 seconds) when your child breathes
Your child’s skin, tongue or lips are blue
Your child feels very cold or clammy to touch
Your child is difficult to wake or to keep awake
Your child has severe pains in their arms, legs neck or back
Your child has a very painful, red area of skin, especially if it is getting bigger quickly
Your baby is under one month old and has a temperature of 38°C
Call 111 or ask for an urgent GP appointment if your child:
The temperature has lasted more than five days
Your child is feeding or eating much less than normal, especially if they are drooling or appear in pain when swallowing
Your baby has had a dry nappy for 12 hours or more or is crying without tears or your child shows other signs of dehydration
feeling thirsty,
dark yellow, strong-smelling pee,
peeing less often than usual,
feeling dizzy or lightheaded,
feeling tired,
a dry mouth, lips and tongue,
sunken eyes (dark circles under eyes)
Your baby is between 1-3 months old and has a temperature of 38°C, or is older than 3 months and has a temperature of 39°C or higher
Your baby feels hotter than usual when you touch their back or chest or feels sweaty
Your child is much more sleepy than normal or irritable (unable to settle them with cuddles, toys, TV, or snacks
Especially if they remain sleepy or irritable despite any fever coming down
Your child has a rash that feels like sandpaper or very red lips or tongue (which may look like a strawberry)
Your child has a fever and a sore throat together with red spots on the roof of their mouth or whitish-yellow spots on the back of their throat and sore lumps under their neck
Your child does not need to be rushed to A&E but you should seek medical advice today.
You can:
- Phone NHS 111 – dial 111
- Ring your GP surgery during their opening usual opening hours
- Contact your nearest Walk-in Centre (click to link find)
Get general advice on the NHS website or from your local Pharmacy if your child:
Treat with paracetamol and ibuprofen if they seem uncomfortable
this lowers the fever and helps the pain
Fever does not need treatment if the child is well
It is simply the body’s way of fighting the bug
Encourage fluids
Ice lollies/lolly-ices work a treat
Most children with a simple sore throat do not need antibiotics
Even in the current climate and will get better on their own
If the fever continues for 5 days, please take them to see their GP.
You can get general advice on the NHS Conditions or from your local pharmacy.